Diabetes is a chronic condition characterized by high blood sugar levels. It primarily comes in two forms: Type 1 and Type 2. Managing diabetes often requires a multifaceted approach, including lifestyle changes, oral medications, and sometimes insulin therapy. Understanding when insulin is needed can help manage the disease effectively and maintain a high quality of life.
What is Insulin?
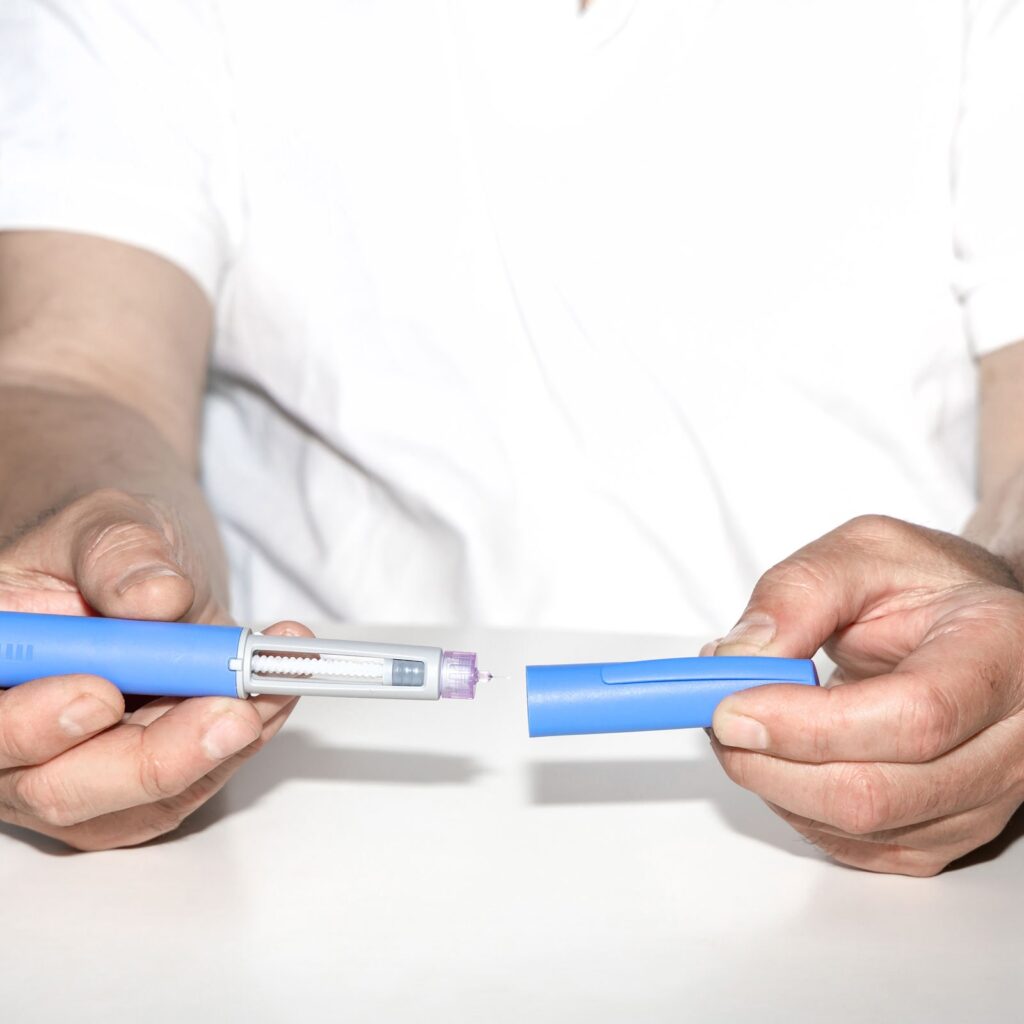
Insulin is a hormone produced by the pancreas that helps regulate blood sugar (glucose) levels. It allows cells to absorb glucose from the bloodstream for energy. In people with diabetes, this process is impaired, leading to elevated blood sugar levels.
Insulin in Type 1 Diabetes
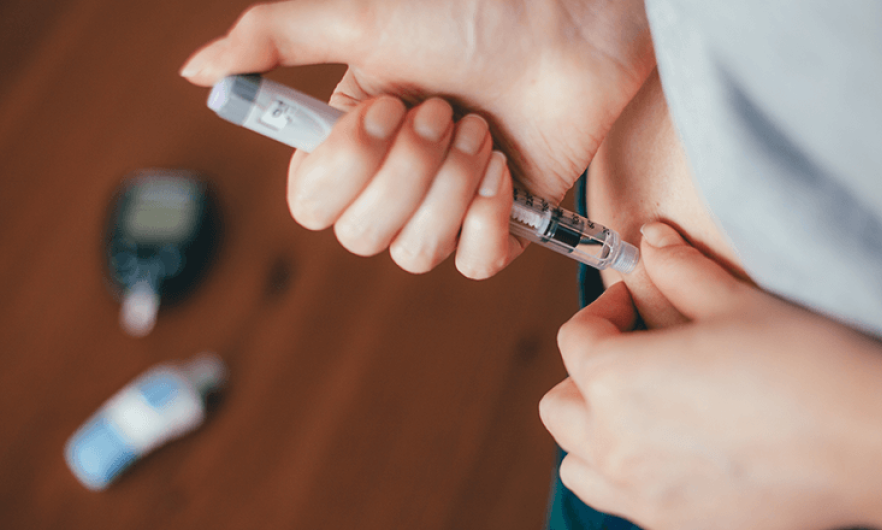
In Type 1 diabetes, the body’s immune system attacks and destroys insulin-producing beta cells in the pancreas. This destruction leads to a complete lack of insulin production. As a result, individuals with Type 1 diabetes need insulin therapy to survive.
Key Points:
- Lack of Insulin Production: Since the pancreas produces little to no insulin, external insulin is essential.
- Daily Management: Insulin is administered through injections or an insulin pump several times a day.
- Blood Sugar Monitoring: Regular blood sugar monitoring is crucial to adjust insulin doses and maintain target levels.
Insulin in Type 2 Diabetes
Type 2 diabetes is characterized by insulin resistance and a relative insulin deficiency. The pancreas produces insulin, but the body’s cells don’t respond effectively to it. Over time, the pancreas may also produce less insulin.
When is Insulin Needed in Type 2 Diabetes?
- Oral Medications Are Insufficient: When lifestyle changes and oral medications fail to control blood sugar levels adequately, insulin may be necessary.
- High Blood Sugar Levels: Persistently high blood sugar levels (hyperglycemia) that don’t respond to other treatments can necessitate insulin.
- During Illness or Surgery: Temporary insulin therapy might be required during periods of acute illness or surgery to better control blood sugar.
- Pregnancy: Women with Type 2 diabetes who become pregnant may need insulin to maintain optimal blood sugar levels for the health of both mother and baby.
- Long-term Diabetes: As Type 2 diabetes progresses, insulin production can decrease, making insulin therapy more likely.
Types of Insulin
There are various types of insulin, classified by how quickly they work and how long they last:
- Rapid-Acting Insulin: Starts working within minutes and lasts a few hours.
- Short-Acting Insulin: Takes effect within 30 minutes and lasts 5-8 hours.
- Intermediate-Acting Insulin: Begins to work in 1-2 hours and lasts up to 18 hours.
- Long-Acting Insulin: Provides a steady level of insulin over 24 hours.
Adjusting to Insulin Therapy

Starting insulin therapy can be daunting, but with the right support and education, it becomes manageable:
- Education: Learning how to administer insulin, understanding dosage, and recognizing signs of high and low blood sugar.
- Support: Working with healthcare providers, diabetes educators, and support groups can help manage the emotional and practical aspects of insulin therapy.
- Technology: Advances like insulin pens, pumps, and continuous glucose monitors (CGMs) make insulin administration easier and more precise.
Conclusion
Insulin is a vital tool in managing diabetes, especially for those with Type 1 diabetes and many with Type 2 diabetes. Recognizing when insulin is needed and how to use it effectively can significantly improve diabetes management and overall quality of life. If you or a loved one is navigating diabetes treatment, consult with healthcare professionals to tailor the best approach for your needs.


